By ,
This article also ran in The Washington Post.
Judith Sullivan was recovering from major surgery at a Connecticut nursing home in March when she got surprising news from h when she got surprising news from her Medicare Advantage plan: It would no longer pay for her care because she was well enough to go home.
At the time, she could not walk more than a few feet, even with assistance — let alone manage the stairs to her front door, she said. She still needed help using a colostomy bag following major surgery.
“How could they make a decision like that without ever coming and seeing me?” said Sullivan, 76. “I still couldn’t walk without one physical therapist behind me and another next to me. Were they all coming home with me?” 
UnitedHealthcare — the nation’s largest health insurance company, which provides Sullivan’s Medicare Advantage plan — doesn’t have a crystal ball. It does have naviHealth, a care management company bought by UHC’s sister company, Optum, in 2020. NaviHealth’s proprietary “nH Predict” tool sifts through millions of medical records to match patients with similar diagnoses and characteristics, including age, preexisting health conditions, and other factors. Based on these comparisons, an algorithm anticipates what kind of care a specific patient will need and for how long.
…Next year, the Centers for Medicare & Medicaid Services will begin restricting how Medicare Advantage plans use predictive technology tools to make some coverage decisions.[Continued on Kaiser Health News and The Washington Post.]…


 The Jan. 25 ruling, which came in response to a 2011 class-action lawsuit eventually joined by 14 beneficiaries against the Department of Health and Human Services, will guarantee p
The Jan. 25 ruling, which came in response to a 2011 class-action lawsuit eventually joined by 14 beneficiaries against the Department of Health and Human Services, will guarantee p







 was a response to complaints from Medicare patients who were surprised to learn that although they had spent a few days in the hospital, they were there for observation and were not admitted. Observation patients are considered too sick to go home yet not sick enough to be admitted. They may pay higher charges than admitted patients and do not qualify for Medicare’s nursing home coverage.
was a response to complaints from Medicare patients who were surprised to learn that although they had spent a few days in the hospital, they were there for observation and were not admitted. Observation patients are considered too sick to go home yet not sick enough to be admitted. They may pay higher charges than admitted patients and do not qualify for Medicare’s nursing home coverage.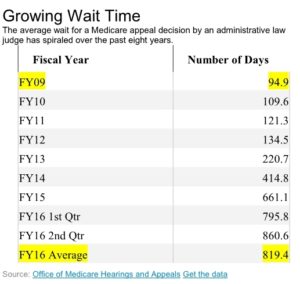 challenging denied claims continues to spiral, increasing the backlog of cases and delaying many decisions well beyond the timeframes set by law, according to a government study released Thursday.
challenging denied claims continues to spiral, increasing the backlog of cases and delaying many decisions well beyond the timeframes set by law, according to a government study released Thursday.
 A disabled senior with serious health problems who successfully challenged Medicare for denying her home health care coverage has racked up another win against the government.
A disabled senior with serious health problems who successfully challenged Medicare for denying her home health care coverage has racked up another win against the government. “I’m very pleased. It makes me feel America is still in good shape.”
“I’m very pleased. It makes me feel America is still in good shape.” 
 Today, A lawsuit filed by fourteen seniors, including seven from Connecticut, seeking Medicare nursing home coverage was dismissed Monday by a federal court judge in Hartford.
Today, A lawsuit filed by fourteen seniors, including seven from Connecticut, seeking Medicare nursing home coverage was dismissed Monday by a federal court judge in Hartford.
 man Services Secretary Kathleen Sebelius. In January, a federal judge approved a settlement in which the government agreed that this “improvement standard” is not necessary to receive coverage.
man Services Secretary Kathleen Sebelius. In January, a federal judge approved a settlement in which the government agreed that this “improvement standard” is not necessary to receive coverage.
