RETIRING Nationwide, hospitals and other providers are leaving private Medicare Advantage plans, putting thousands of seniors at risk of higher costs and of losing trusted doctors.
By
Amy Trojanowski liked the extra benefits her Humana Medicare Advantage plan provided — a $200 debit card replenished monthly to use toward groceries, over-the-counter pharmacy items and even her electric bill. She also appreciated the dental and vision coverage. But those things couldn’t compare to the doctor she had been seeing for nearly a decade.![]()
“I love her so much,” said Ms. Trojanowski, 60, who lives near Raleigh, N.C. The doctor’s practice is part of UNC Health, a 20-hospital system affiliated with the University of North Carolina at Chapel Hill.
Last October, however, Humana informed her that UNC Health would no longer participate in the plan’s provider network in 2026….
In November, the Centers for Medicare & Medicaid Services proposed a regulation with a solution for Advantage members “who experience provider network changes midyear” and “may want to stay with their current provider,” according to a C.M.S. fact sheet. Officials would streamline a complicated process “to allow these enrollees to change their coverage more easily.” State insurance officials, the American Medical Association and the American Hospital Association, along with other provider and patient advocacy groups, generally supported the idea.
But early this month, C.M.S. abandoned the proposal, which would have taken effect in 2027, even as disruptions in provider networks continue. C.M.S. officials declined to explain the reason for the reversal. But in an email, a C.M.S. spokesman, Christopher Krepich, wrote that the agency “routinely proposes policies to solicit public input and carefully considers all feedback” before finalizing them. [Continued in The New York Times.]…








 was a response to complaints from Medicare patients who were surprised to learn that although they had spent a few days in the hospital, they were there for observation and were not admitted. Observation patients are considered too sick to go home yet not sick enough to be admitted. They may pay higher charges than admitted patients and do not qualify for Medicare’s nursing home coverage.
was a response to complaints from Medicare patients who were surprised to learn that although they had spent a few days in the hospital, they were there for observation and were not admitted. Observation patients are considered too sick to go home yet not sick enough to be admitted. They may pay higher charges than admitted patients and do not qualify for Medicare’s nursing home coverage.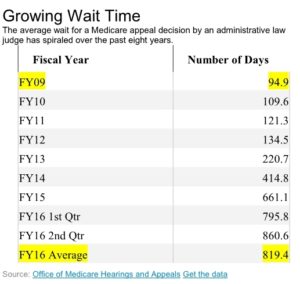 challenging denied claims continues to spiral, increasing the backlog of cases and delaying many decisions well beyond the timeframes set by law, according to a government study released Thursday.
challenging denied claims continues to spiral, increasing the backlog of cases and delaying many decisions well beyond the timeframes set by law, according to a government study released Thursday.




