 Volume 399, Issue 10323
Volume 399, Issue 10323
28 January 2022
WORLD REPORT As the Supreme Court blocks one of the Biden Administration’s plans to raise COVID-19 vaccination rates but approves another, Susan Jaffe looks at the next steps.
…
 Volume 399, Issue 10323
Volume 399, Issue 10323
WORLD REPORT As the Supreme Court blocks one of the Biden Administration’s plans to raise COVID-19 vaccination rates but approves another, Susan Jaffe looks at the next steps.
…
 Volume 399, Issue 10321
Volume 399, Issue 10321
WORLD REPORT The founder of Theranos was found guilty of defrauding some investors, but cleared of charges that she misled patients. Susan Jaffe reports.
 Volume 398, Issue 10315
Volume 398, Issue 10315
 Volume 398, Issue 10314
Volume 398, Issue 10314
WORLD REPORT Almost a year after the first COVID-19 vaccine was approved for emergency use in the USA, roughly a third of adults have still not received it. After urging Americans to get vaccinated, US President Joe Biden has taken a tougher approach: under his administration’s new workplace safety standard, people must get vaccinated or undergo weekly tests for the virus if they work for companies with at least 100 employees. “The rule will protect more than 84 million workers from the spread of the coronavirus on the job”, said Jim Frederick, Deputy Assistant Secretary of Labor for Occupational Safety and Health. …A day after OSHA’s announcement on Nov 4, 2021, multiple lawsuits to block the rule started rolling in to federal courts across the country.[Continued here.]
…

In response, the Centers for Medicare and Medicaid Services has threatened to penalize private insurance companies selling Medicare Advantage and drug plans if they or agents working on their behalf mislead consumers. The agency has also revised rules making it easier for beneficiaries to escape plans they didn’t sign up for or enrolled in only to discover promised benefits didn’t exist or they couldn’t see their providers.
The problems are especially prevalent during Medicare’s open-enrollment period, which began Oct. 15 and runs through Dec. 7. A common trap begins with a phone call like the one Linda Heimer, an Iowa resident, received in October. [Full story in The Washington Post and Kaiser Health News.]
Nursing homes receive billions of taxpayers’ dollars every year to care for chronically ill frail elders, but until now, there was no guarantee that’s how the money would be spent.
Massachusetts, New Jersey and New York are taking unprecedented steps to ensure they get what they pay for, ![]() after the devastating impact of covid-19 exposed problems with staffing and infection control in nursing homes. The states have set requirements for how much nursing homes
after the devastating impact of covid-19 exposed problems with staffing and infection control in nursing homes. The states have set requirements for how much nursing homes  must spend on residents’ direct care and imposed limits on what they can spend elsewhere, including administrative expenses, executive salaries and advertising and even how much they can pocket as profit. …With this strategy, advocates believe, residents won’t be shortchanged on care, and violations of federal quality standards should decrease because money will be required to be spent on residents’ needs. At least that’s the theory. [Continued on Kaiser Health News, Fortune, NBC News, Yahoo Finance, and Chicago Sun-Times]…
must spend on residents’ direct care and imposed limits on what they can spend elsewhere, including administrative expenses, executive salaries and advertising and even how much they can pocket as profit. …With this strategy, advocates believe, residents won’t be shortchanged on care, and violations of federal quality standards should decrease because money will be required to be spent on residents’ needs. At least that’s the theory. [Continued on Kaiser Health News, Fortune, NBC News, Yahoo Finance, and Chicago Sun-Times]…
 Sept. 20, 2021 | Today on NPR‘s news program “1A,” reporter Susan Jaffe discusses her Kaiser Health News story about new state laws protecting nursing home residents in response to the COVID-19 pandemic. Changes affect staffing, visitation rights, virtual communications, “essential support persons,” and more. A resident of a Connecticut nursing home quoted in this KHN article is also a guest. …
Sept. 20, 2021 | Today on NPR‘s news program “1A,” reporter Susan Jaffe discusses her Kaiser Health News story about new state laws protecting nursing home residents in response to the COVID-19 pandemic. Changes affect staffing, visitation rights, virtual communications, “essential support persons,” and more. A resident of a Connecticut nursing home quoted in this KHN article is also a guest. …
So far, 23 states have passed more than 70 new pandemic-related provisions affecting nursing home operations.
By Susan Jaffe | KAISER HEALTH NEWS | August 17, 2021 | This story also ran in![]()
When the coronavirus hit Martha Leland’s Connecticut nursing home last year, she and dozens of other residents contracted the disease while the facility was on lockdown. Twenty-eight residents died, including her roommate.
“The impact of not having friends and family come in and see us for a year was totally devastating,” she said. “And then, the staff all bound up with the masks and the shields on, that too was very difficult to accept.” She summed up the experience in one word: “scary.”
But under a law Connecticut enacted in June, nursing home residents will be able to designate an “essential support person” who can help

take care of a loved one even during a public health emergency. Connecticut legislators also approved laws this year giving nursing home residents free internet access and digital devices for virtual visits and allowing video cameras in their rooms so family or friends can monitor their care.
Similar benefits are not required by the Centers for Medicare & Medicaid Services, the federal agency that oversees nursing homes and pays for most of the care they provide. But states can impose additional requirements when those federal rules are insufficient or don’t exist. And that’s exactly what many are doing, spurred by the virus that hit the frail elderly hardest. [Continued at Kaiser Health News and USA Today]
…
 Volume 398, Issue 10300
Volume 398, Issue 10300

…
By Susan Jaffe | Kaiser Health News | June 9, 2021 | This KHN story also ran on![]() and
and
Patty Bausch isn’t a Medicaid expert, lawyer or medical professional. But she still thinks Connecticut legislators need her input when they consider bills affecting people like her — the roughly 18,000 residents who live in the state’s nursing homes.
With help and encouragement from Connecticut’s Long Term Care Ombudsman Program, Bausch signed up and testified remotely before a legislative hearing this year. Nursing home residents who have been using digital technology to reach out to family and friends — after the covid pandemic led officials to end visitation last year — could also use it to connect with elected officials once the legislature moved to remote hearings. Speaking into an iPad provided by the ombudsman’s office, Bausch testified without ever leaving her room at the Newtown Rehabilitation & Health Care Center, where she has lived since having a stroke three years ago. The combination of a virtual legislature and nursing home residents equipped with internet access has created an opportunity most nursing home residents rarely have — to participate in their government up close and in real time. [Continued on Kaiser Health News, Next Avenue and Connecticut Public Radio.]…
 rgeries so risky for older adults that that the insurance program would cover the procedures only for patients admitted to the hospital. Under a new Medicare policy that took effect this year, these operations can be provided to patients who are not admitted. But patients still have to go to the hospital. The change saves Medicare money while patients can pay a larger share of the bill — for the same surgery at the same hospital. [Full story in The Washington Post and Kaiser Health News.]
rgeries so risky for older adults that that the insurance program would cover the procedures only for patients admitted to the hospital. Under a new Medicare policy that took effect this year, these operations can be provided to patients who are not admitted. But patients still have to go to the hospital. The change saves Medicare money while patients can pay a larger share of the bill — for the same surgery at the same hospital. [Full story in The Washington Post and Kaiser Health News.] 
By narrowly approving a massive COVID-19 response and economic relief package last week, Democrats in Congress handed President Joe Biden his first legislative victory after only 50 days in the White House. The US$1·9 trillion, 628-page, American Rescue Plan Act is a signature achievement so monumental that it has been compared to President Lyndon B Johnson’s sweeping Great Society legislation that raised many Americans out of poverty, with a safety net of social and health services, including the Medicare and Medicaid insurance programmes.
…As the government begins to roll out these benefits, Biden promised “fastidious oversight to make sure there’s no waste or fraud, and the law does what it’s designed to do. And I mean it: we have to get this right… because we have to continue to build confidence in the American people that their government can function for them and deliver.” [Full story with “where the money goes” sidebar here.]
…
COVID-19 has rampaged through nursing homes and other long-term-care facilities, leaving a death toll near 180,000 and counting. So when the first coronavirus vaccines became available at the end of last year, nursing home residents and staff were first in line, given top priority along with emergency responders and health care providers.
![]()
The federal government paid CVS and Walgreens to offer three vaccination clinics for residents and staff at nearly every nursing home in the U.S. That effort, called the Pharmacy Partnership for Long-Term Care Program, wraps up this month. So how do new nursing home residents and workers who missed the onsite clinics get vaccinated now? For residents, plans are in the works to make sure they get the shots. But so far, many of those plans don’t include the staff members who care for them. [Continued here.]…
By Susan Jaffe | Contributing Writer | MedPageToday | November 25, 2020

More than 91,000 residents and staff of long-term care facilities have died after contracting COVID-19 — about 40% of the total deaths in the U.S., according to a Kaiser Family Foundation analysis. …Frustrated by repeated violations of infection control requirements during the pandemic, CMS raised the penalty amounts and announced a crackdown on egregious offenders in August. But the hard-line approach doesn’t seem to have produced the intended results. (Click here for a list of nursing homes that were fined.) [Continued here.]
Seniors would be notified about eligibility to avoid late fees, coverage gap
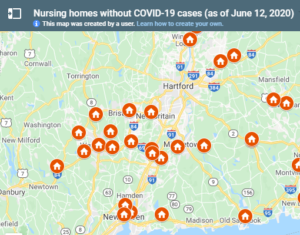

More than 600 residents have died from COVID-19 at 25 New York City nursing homes that received clean bills of health for controlling the spread of infections, state Department of Health inspection reports obtained by THE CITY show.
Those facilities inclu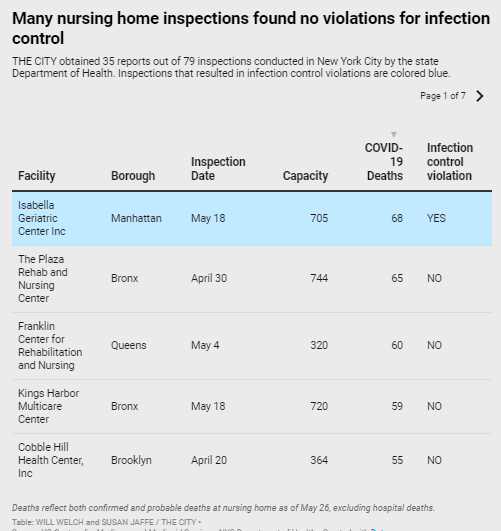 de homes with some of the highest coronavirus death tolls in the nation — including the Sapphire Center for Rehabilitation and Nursing in Flushing, which reports 54 residents died of confirmed or presumed COVID….
de homes with some of the highest coronavirus death tolls in the nation — including the Sapphire Center for Rehabilitation and Nursing in Flushing, which reports 54 residents died of confirmed or presumed COVID….
At the Franklin Center for Rehabilitation and Nursing, also in Flushing, 60 residents — nearly one in five — succumbed to the virus. Its May 4 inspection report found no problems.
Also passing its May 11 infection-control inspection was New York State Veterans Home in St. Albans, Queens. Staff there previously told THE CITY that the state Health Department-run home failed to separate COVID-positive and uninfected residents, something that was a violation at other facilities….
“It’s very shocking that at the apex of this pandemic, our inspectors went in and reported that that there’s nothing out of the ordinary when it’s clear that the infection rate had spread,” said Assemblymember Ron Kim (D-Queens), whose district includes Sapphire and the Franklin Center. [continued here].
…
By

Eyes and ears usually trained on New York’s nursing homes and adult care facilities have been nearly locked out as the coronavirus has claimed the lives of more than 3,500 residents statewide.

Almost entirely out of the picture are nursing home inspectors,employed by the state Department of Health and
coordinated by the federal government, who are responsible for ensuring that the facilities comply with federal health and safety requirements.
“Nursing facilities are essentially free of public scrutiny right now, at a time when scrutiny is more important than ever,” said Susan Dooha, executive director of the Center for Independence of the Disabled in New York [continued here].
…
As coronavirus cases increase, posing heightened risks to the elderly, nursing homes will face growing scrutiny from state health inspectors.
In Connecticut and nationally, complying with federal infection-control requirements is a challenge for some nursing homes. Between 2017 and 2019, 145 of Connecticut’s 217 nursing homes – or about 67 percent – were cited for infection-control violations, according to a Conn. Health I-Team analysis of data from the Centers for Medicare & Medicaid Services (CMS). [Continued here, with list of nursing home infection violations.]
…
Current enrollment rules can leave late enrollees liable for doc visits Medicare usually covers
Saturday is the deadline for most people with Medicare coverage to sign up for private drug and medical plans for next year. But members of Congress, heal th care advocates and insurance agents worry that enrollment decisions based on bad information from the government’s revamped, error-prone Plan Finder website will bring unwelcome surprises.
th care advocates and insurance agents worry that enrollment decisions based on bad information from the government’s revamped, error-prone Plan Finder website will bring unwelcome surprises.
Beneficiaries could be stuck in plans that cost too much and don’t meet their medical needs — with no way out until 2021.
On Wednesday, the Centers for Medicare & Medicaid Services told Kaiser Health News that beneficiaries would be able to change plans next year because of Plan Finder misinformation, although officials provided few details. [Continued at Kaiser Health News or NPR.] …
By Susan Jaffe | Kaiser Health News | October 8, 2019 | This article also ran in the![]()
Millions of older adults can start signing up next week for private policies offering Medicare drug and medical  coverage for 2020. But many risk wasting money and even jeopardizing their health ca
coverage for 2020. But many risk wasting money and even jeopardizing their health ca![]() re due to changes in Medicare’s plan finder, its most popular website.
re due to changes in Medicare’s plan finder, its most popular website.
For more than a decade, beneficiaries used the plan finder to compare dozens of Medicare policies offered by competing insurance companies and get a list of their options. Yet after a website redesign six weeks ago, the search results are missing crucial details: How much will you pay out-of-pocket? And which plan offers the best value? [Continued at Kaiser Health News, San Francisco![]()
By Susan Jaffe | Kaiser Health News | August 12, 2019 | This KHN story also ran on Salon and Next Avenue
Medicare paid for Betty Gordon’s knee replacement surgery in March, but the 72-year-old former high school teacher needed a nursing home stay and care at home to recover.
![]()
Yet Medicare wouldn’t pay for that. So Gordon is stuck with a $7,000 bill she can’t afford — and, as if that were not bad enough, she can’t appeal.

The reasons Medicare won’t pay have frustrated the Rhode Island woman and many others trapped in the maze of regulations surrounding something called “observation care.”
Patients, like Gordon, receive observation care in the hospital when their doctors think they are too sick to go home but not sick enough to be admitted. They stay overnight or longer, usually in regular hospital rooms, getting some of the same services and treatment (often for the same problems) as an admitted patient….

(Photo courtesy of Betty Gordon)
But observation care is considered an outpatient service under Medicare rules, like a doctor’s appointment or a lab test. Observation patients may have to pay a larger share of the hospital bill than if they were officially admitted to the hospital.Medicare’s nursing home benefit is available only to those admitted to the hospital for three consecutive days. Gordon spent three days in the hospital after her surgery, but because she was getting observation care, that time didn’t count.

There’s another twist: Patients might want to file an appeal, as they can with many other Medicare decisions. But that is not allowed if the dispute involves observation care.
Monday, a trial begins in federal court in Hartford, Conn., where patients who were denied Medicare’s nursing home benefit are hoping to force the government to eliminate that exception. A victory would clear the way for appeals from hundreds of thousands of people. [Continued at Kaiser Health News, Next Avenue or Salon]
…