By Susan Jaffe | Kaiser Health News | May 2, 2017 | This KHN story also ran in 
Since retiring four years ago, Barbara Corprew has visited Paris, traveled to a North Carolina film festival and taken Pilates classes, focusing on — as she puts it — just “doing things for me.” Now the former Justice Department lawyer, who worked on white-collar crime cases, is devoting time to something completely different: She visits nursing homes every week.

Barbara Corprew, says her service as a volunteer ombudsman was sparked in part by her experience acting as an advocate for her parents when they became ill. (Courtesy of Barbara Corprew)
Corprew is a volunteer in the District of Columbia’s Long-Term Care Ombudsman’s Office, a government-funded advocacy agency for nursing home and assisted-living residents.
The ombudsmen’s offices, which operate under federal law in all 50 states and the District, investigated 200,000 complaints in 2015, according to the Administration on Aging, a part of the Department of Health and Human Services. Of those, almost 117,000 were reported to have been resolved in a way that satisfied the person who made the complaint, and about 30,000 were partially resolved. At the top of the list were problems concerning care, residents’ rights, physical environment, admissions and discharges, and abuse and neglect.
The volunteers have permission to enter any nursing home, assisted-living or other long-term-care facility anytime, unannounced, talk to any resident and go wherever they want. They respond to issues raised by residents and their families and can bring up problems they discover. All complaints are handled confidentially, even kept from family members, unless residents allow the ombudsman to reveal their identities.
… Medical or legal experience is not required. Volunteers come from all kinds of backgrounds and careers, but they seem to have one thing in common: an abundance of compassion.
Gwendolyn Devore, another District volunteer, remembers a forlorn woman sitting in a hallway at the nursing home where her aunt lived. When she asked a staff member about the woman, the only reply was an angry look that unmistakably said, “It’s none of your business,” Devore recalled as she explained her interest in becoming a volunteer. “Now no one will be able to say it’s none of my business.” [Continued at Kaiser Health News and in The Washington Post]…




 When Christine Williams began working as a nurse practitioner some forty years ago in
When Christine Williams began working as a nurse practitioner some forty years ago in 





 and
and  noticed an uptick in mail solicitations from health insurance companies, which can mean only one thing: It’s time for the annual Medicare open enrollment.
noticed an uptick in mail solicitations from health insurance companies, which can mean only one thing: It’s time for the annual Medicare open enrollment.

 as people who have qualified for Medicare due to a disability but chose to use marketplace plans.
as people who have qualified for Medicare due to a disability but chose to use marketplace plans. 

 reschool teacher who lives in Kingsley Manor, a retirement community in Los Angeles. “I didn’t know what I was going to do about dental care.”
reschool teacher who lives in Kingsley Manor, a retirement community in Los Angeles. “I didn’t know what I was going to do about dental care.”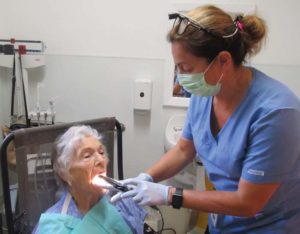
 nis, acting director of the Medicare Enrollment and Appeals Group at the Centers for Medicare & Medicaid Services.
nis, acting director of the Medicare Enrollment and Appeals Group at the Centers for Medicare & Medicaid Services. 
 Looking for ways to save money and improve care, Medicare officials are returning to an old-fashioned idea: house calls.
Looking for ways to save money and improve care, Medicare officials are returning to an old-fashioned idea: house calls.

 fractured hips and head injuries to irreversible calamities that can lead to death.
fractured hips and head injuries to irreversible calamities that can lead to death.
